A short documentary was filmed about last year's mental health rally by Brave New Films! It was an amazing experience.
Check out the video. ⤵

Discover Monthly
Obsessive-Compulsive Disorder
(OCD)
What is OCD?
According to the International OCD Foundation
Obsessive compulsive disorder (OCD) is a mental health disorder that affects people of all ages and walks of life, and occurs when a person gets caught in a cycle of obsessions and compulsions. Obsessions are unwanted, intrusive thoughts, images, or urges that trigger intensely distressing feelings. Compulsions are behaviors an individual engages in to attempt to get rid of the obsessions and/or decrease his or her distress.
Different Types of OCD:
According to TreatMyOCD.com, VeryWellMind.com, and Gateway OCD
-
Contamination Obsessions
-
Contamination OCD is probably the most stereotyped form of OCD. People with this subtype are afraid of getting sick, or infecting someone they care about, after coming in contact with serious bacteria.
-
-
Harm Obsessions with Checking Compulsions
-
Harm OCD causes people to be deeply disturbed by the violent thoughts that just about everyone has experienced. While most people are able to shrug off these thoughts, those with Harm OCD can become completely overwhelmed by them.
-
-
Symmetry Obsessions
-
People who suffer from Symmetry OCD become fixated on the position and arrangement of certain objects and will feel uncomfortable and distressed when encountering items that are not aligned correctly or that or appear somehow incomplete. People with this form of OCD will struggle when words they write appear in an undesirable shape or are not perfectly positioned along the line.
-
-
Sexual Orientation OCD
-
Sexual Orientation OCD (Homosexual OCD or HOCD) involves obsessions about one’s sexuality. It’s often called Homosexual OCD, but this is misleading. It can happen to people of any sexuality, about any other sexuality.
-
-
Pedophilia OCD
-
Pedophilia OCD is especially prone to stigma because of how strong people’s feelings are about pedophiles. However, as with all types of OCD, these obsessions are not desires. In fact, people are so distressed by these thoughts because they don’t reflect what they really want.
-
-
Relationship OCD
-
Relationship OCD leaves people completely unable to tolerate the uncertainty of intimate relationships, giving them obsessions about the “rightness” of their own relationship and the countless other possibilities that daily life brings.
-
-
“Just Right” OCD
-
“Just Right” OCD is a little different from these other subtypes, in that it’s difficult to identify a specific fear, or set of fears, underlying it. Instead, it’s usually more like a strong feeling that something just isn’t right when things aren’t a certain way. It’s one of the more caricatured forms of OCD, in TV shows, movies, and jokes.
-
-
Pure-O
-
Pure-O, or Pure Obsessional OCD, is one of the murkier subtypes, and some experts say it doesn’t even exist. The idea is that people with Pure-O have obsessions without visible compulsions, but since they still have compulsions they’re not exactly “purely obsessional.” But whether or not studies back it, many people identify with Pure-O because they don’t have the more obvious compulsions listed in subtypes above. The obsessions can be about sex, sexuality, religion, harm, personal health, romance, and really anything else we discussed above.
-
General Statistics
According to the NIMH
-
Based on diagnostic interview data from the National Comorbidity Survey Replication (NCS-R), Figure 1 shows past year prevalence of OCD among U.S. adults aged 18 or older.
-
Past year prevalence of OCD was higher for females (1.8%) than for males (0.5%).
-
-
An estimated 1.2% of U.S. adults had OCD in the past year.
-
Lifetime prevalence of OCD among U.S. adults was 2.3%.
What is OCD?
View full lesson: http://ed.ted.com/lessons/debunking-t...
There’s a common misconception that if you like to meticulously organize your things, keep your hands clean, or plan out your weekend to the last detail, you might be OCD. In fact, OCD (Obsessive Compulsive Disorder) is a serious psychiatric condition that is frequently misunderstood by society and mental health professionals alike. Natascha M. Santos debunks the myths surrounding OCD.
Lesson by Natascha M. Santos, animation by Zedem Media.
ARTICLES ABOUT OBSESSIVE COMPULSIVE DISORDER
Obsessive-Compulsive Disorder Is No Joke
By Emily Dixon
"The biggest lie about Obsessive-Compulsive Disorder is that it’s funny, though it is, at times. I laugh when I remember running for the school bus barefoot every morning, brandishing my shoes and socks to flag down the driver, because I had to button and unbutton my uniform so many times — in multiples of four — that I could never quite find the time to clothe my feet."

A Look Inside My World With OCD
By Stacey Frewin
"A seemingly 'normal' day can flip in an instant. A single touch, thought or action can change everything. A loss of control if only for a moment can unravel your entire day, consumed by a singular feeling: fear. Many people experience fear, but in some people, fear isn’t just a worry — it consumes every thought and action. Fear doesn’t discriminate: age, race, sexuality or religion, we will all fear “true” fear at some point in our lives. This is what living with obsessive-compulsive disorder (OCD) is like."

Quirks That Made More Sense Once I Was Diagnosed With OCD
By Amanda Dodson Gremillion
"When I was a child I would often count how many steps it took to get across a room (or to a certain point in a room), or outside or in a parking lot and would often try to make it across or to those certain points in a certain amount of steps. I even thought maybe if I accomplished this, I would somehow have good luck or something. And if I did not, maybe something bad would happen... These things are just a couple of the quirks I did not realize at first might be symptoms of obsessive-compulsive disorder (OCD). At first, I thought everyone just did this."

THE
CHEMISTRY
BEHIND OCD
Most mental illnesses have been tied in some way to the chemicals in the brain or to alterations in activity or structures in the brain. Neurotransmitters, the chemicals that are used as signaling molecules between neurons, play a big role in many conditions, like depression, anxiety disorders, and OCD. Changes, deficiencies, or other abnormalities in these chemicals certainly play a role in many mental illnesses. Brain chemistry has long been an area of study for researchers trying to determine what causes OCD.
Serotonin is a prime candidate for a potential cause or contributing factor to OCD. Antidepressant medications that increase the amount of serotonin in the brain, called SSRIs, work well for most people with OCD. This may mean that a deficiency in serotonin contributes to OCD, although it is probably not the single cause for any one person with the condition.
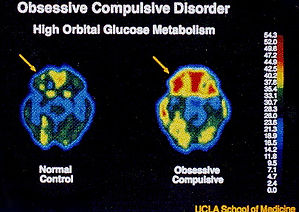
With imaging scans of the brain, researchers have been able to determine that there are three areas or structures in the brain that are more active in people with OCD. This further indicates that brain abnormalities are implicated as contributing causes. The three areas of the brain that are overactive are:
-
The caudate nucleus. This part of the brain is associated with filtering thoughts and managing habits. When OCD is well managed with treatment, activity in this area goes down.
-
The prefrontal orbital cortex. This area is associated with managing appropriate social behaviors. Decreased activity here leads to lowered inhibitions, but increased activity can cause social anxiety and worries about cleanliness or acting inappropriately.
-
The cingulate gyrus. Located in the center of the brain, this region is thought to regulate how a person reacts to troubling thoughts and obsessions. Over-activity here may trigger compulsive behaviors.
The most recent OCD research has implicated yet another brain chemistry factor that could explain the condition. Researchers working with laboratory mice investigated a protein called SPRED2. Found in all cells in the body, it is especially concentrated in the brain. When the protein was eliminated from the mice, it triggered compulsive and excessive grooming. The researchers hope that by targeting this protein and the chemical pathways it triggers, they can develop a better treatment for OCD.
SPRED2 Gene
HOW DOES TREATMENT HELP?
"Treatment for most OCD patients should involve Exposure and Response Prevention (ERP) and/or medication. The majority of people with OCD (about 7 out of 10) will benefit from either medication or ERP.
What Are the Most Effective Treatments for OCD?
The most effective treatments for OCD are Cognitive Behavior Therapy (CBT) and/or medication. [1] More specifically, the most effective treatments are a type of CBT called Exposure and Response Prevention (ERP), which has the strongest evidence supporting its use in the treatment of OCD, and/or a class of medications called serotonin reuptake inhibitors, or SRIs.
Exposure and Response Prevention is typically done by a licensed mental health professional (such as a psychologist, social worker, or mental health counselor) in an outpatient setting. This means you visit your therapist’s office at a set appointment time once or a few times a week.
Medications can only be prescribed by a licensed medical professionals (such as your physician or a psychiatrist), who would ideally work together with your therapist to develop a treatment plan.
Taken together, ERP and medication are considered the “first-line” treatments for OCD. In other words, START HERE! About 70% of people will benefit from ERP and/or medication for their OCD.
What if Outpatient ERP Hasn’t Worked? Are There More Intensive Options?
Yes. If you or a loved one has tried traditional outpatient therapy and would like to try a more intensive level of care, there are options. The IOCDF keeps a Resource Directory of intensive treatment centers, specialty outpatient clinics, and therapist who provide these various levels of services for OCD. The following lists therapy options from least intensive to most intensive:
Traditional Outpatient
Patients see a therapist for individual sessions as often as recommended by their therapist generally one or two times a week for 45-50 minutes. (Most Therapists in the Resource Directory as well as “Specialty Outpatient Clinics” offer this type of treatment).
Intensive Outpatient
Patients may attend groups and one individual session per day several days per week. Clinics designated as “Intensive Treatment Programs” in the Resource Directory offer this level of treatment.
Day Program
Patients attend treatment during the day (typically group and individual therapy) at a mental health treatment center usually from 9am – 5pm up to five days a week. Many clinics designated as “Intensive Treatment Programs” in the Resource Directory offer this level of treatment.
Partial Hospitalization
Same as the Day Program but patients attend the treatment at a mental health hospital. Several clinics designated as “Intensive Treatment Programs” in the Resource Directory offer this level of treatment.
Residential
Patients are treated while living voluntarily in an unlocked mental health treatment center or hospital. Clinics designated as “Residential” in the Resource Directory offer this level of treatment.
Inpatient
This is the highest level of care for a mental health condition. Treatment is provided on a locked unit in a mental health hospital on a voluntary or sometimes involuntary basis. Patients are admitted into this level of care if they are unable to care for themselves or are a danger to themselves or others. The goals of inpatient treatment are to stabilize the patient, which generally takes several days to a week, and then transition the patient to a lower level of care.
Additional Treatment Options for OCD
Other recommendations from the APA Practice Guideline,1 cite research showing that ERP delivered in a group format, as well as ERP therapy delivered via videoconferencing (teletherapy), might be effective. Also, there is some promising new research showing that Acceptance and Commitment Therapy may be helpful for OCD.."
HOW TO HELP SOMEONE YOU KNOW STRUGGLING:
"Finally, after years of not knowing where to turn, someone has given it a name. A family member has been diagnosed as having Obsessive Compulsive Disorder (OCD) and you want to learn all you can about the disorder. Caring about your loved one with OCD, you have undoubtedly wondered “What can I do to help?”
Become educated about OCD
Education is the first step. Learn as much about OCD as you can: read books, join the Obsessive Compulsive Foundation (www.ocfoundation.org), find out if the state you live in has an OCF affiliate, attend OCD support groups, research online, etc. As you learn more about the disorder, you begin to feel hopeful that you can do things to help the person with OCD overcome their disorder. OCD is a biochemically-based disorder with clinical symptoms that go beyond personality traits. As your understanding increases, you will be able to view the irrational behaviors from a non-personalized perspective. If you have been neglecting yourself, engage in self-care that will impact your ability to problem solve and respond to your family member more constructively. Your family relationships will improve and the person with OCD will feel more supported. Positive family relationships and feeling understood greatly enhance the therapeutic benefits of treatment.
Learn to recognize and reduce “Family Accommodation"
Families are constantly affected by the demands of OCD. Results from research investigating family and OCD suggest that family responses may play a role in maintaining or even facilitating OCD symptoms. The more that family members can learn about their responses to OCD and the impact that their responses have on the person with OCD, the more the family becomes empowered to make a difference! Consider the following responses you might engage in when responding to your family member’s struggle with OCD symptoms.
Help your family member find appropriate, effective treatment by a qualified professional
Experienced clinicians agree that a multimodal treatment approach that includes medication, behavior therapy, and family education and support is optimal.
Learn strategies about how to respond if your family member refuses treatment
Sometimes, when the discomfort or impairment becomes so great that it affects a job, relationships, enjoyment of life, the person with OCD will come forward to accept professional advice. Families have told me of watching the bottom “fall out” and just how badly things deteriorated before their loved one would admit to a problem. This is a painful process and you have choices as a support person. Often admission to “a problem” does not mean acceptance of the problem or giving into it; admission is the first step in being able to identify that the person has a legitimate neurobiological disorder with distinct treatment, rather than the problems stemming from character flaws. For the whole family acceptance is a process that takes time."
If your loved one is a danger to themselves or others, seek help right away:
-
Call 911 for emergency services or go to the closet emergency room
-
Call the National Suicide Prevention Lifeline (Lifeline) at 899 or text the Crisis Text Line (text HELLO to 741741)
BOOKS THAT EFFECTIVELY PORTRAY OCD

Every Last Word
by Tamara Ireland Stone
Overview
"Samantha McAllister looks just like the rest of the popular girls in her junior class. But hidden beneath the straightened hair and expertly applied makeup is a secret that her friends would never understand: Sam has Purely-Obsessional OCD and is consumed by a stream of dark thoughts and worries that she can't turn off."

History Is All You Left Me
by Adam Silvera
Overview
"When Griffin's first love and ex-boyfriend, Theo, dies in a drowning accident, his universe implodes. Even though Theo had moved to California for college and started seeing Jackson, Griffin never doubted Theo would come back to him when the time was right. But now, the future he's been imagining for himself has gone far off course."

The Unlikely Hero of Room 13B
by Teresa Toten
Overview
"When Adam meets Robyn at a support group for kids coping with obsessive-compulsive disorder, he is drawn to her almost before he can take a breath. He's determined to protect and defend her--to play Batman to her Robyn--whatever the cost. But when you're fourteen and the everyday problems of dealing with divorced parents and step-siblings are supplemented by the challenges of OCD, it's hard to imagine yourself falling in love. How can you have a "normal" relationship when your life is so fraught with problems? And that's not even to mention the small matter of those threatening letters Adam's mother has started to receive . . ."
CELEBRITIES WHO ADVOCATE

"In an interview Leonardo recalled how he let his OCD symptoms go, and how this quickly worsened his OCD. He explains, “I remember my make-up artist and assistant walking me to the set and going, ‘Oh, God, here he goes again. We’re going to need 10 minutes to get him to the set today because he has to walk back and step on that thing and touch the door in a certain way and then walk in and walk out again.’ I let myself do it because I wanted that to come out.”

"Singer and actor Justin Timberlake has said that he suffers from both attention-deficit disorder and obsessive-compulsive disorder. "You try living with that," he laments. "It's complicated." Timberlake's OCD behaviors include an obsession with lining objects up and feeling that he absolutely must have a certain food item in the house at all times."

.png)
.png)

